Small Intestine
Lesson 4 of 16 · Detailed theory + identification points
Points of Identification
4 pointsDetailed Theory
Object: Examination of Histological Slide of Small Intestine
General Overview
The small intestine is the principal site of digestion and nutrient absorption, extending ~6–7 m from the pylorus to the ileocaecal valve. It is divided into duodenum (25 cm), jejunum (~2.5 m), and ileum (~3.5 m). Its enormous absorptive surface area is achieved through three structural adaptations: plicae circulares, villi, and microvilli (brush border).
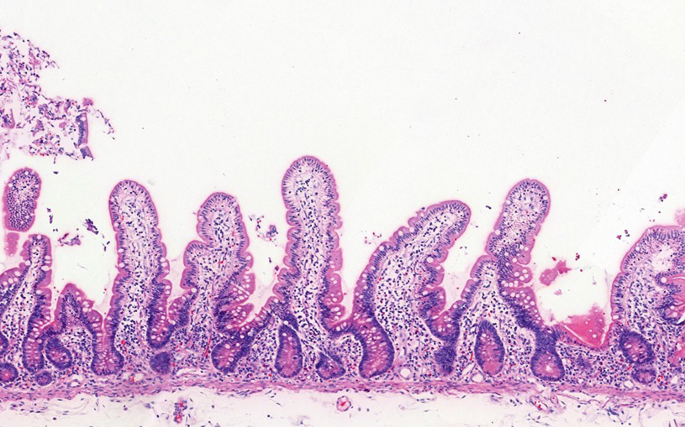
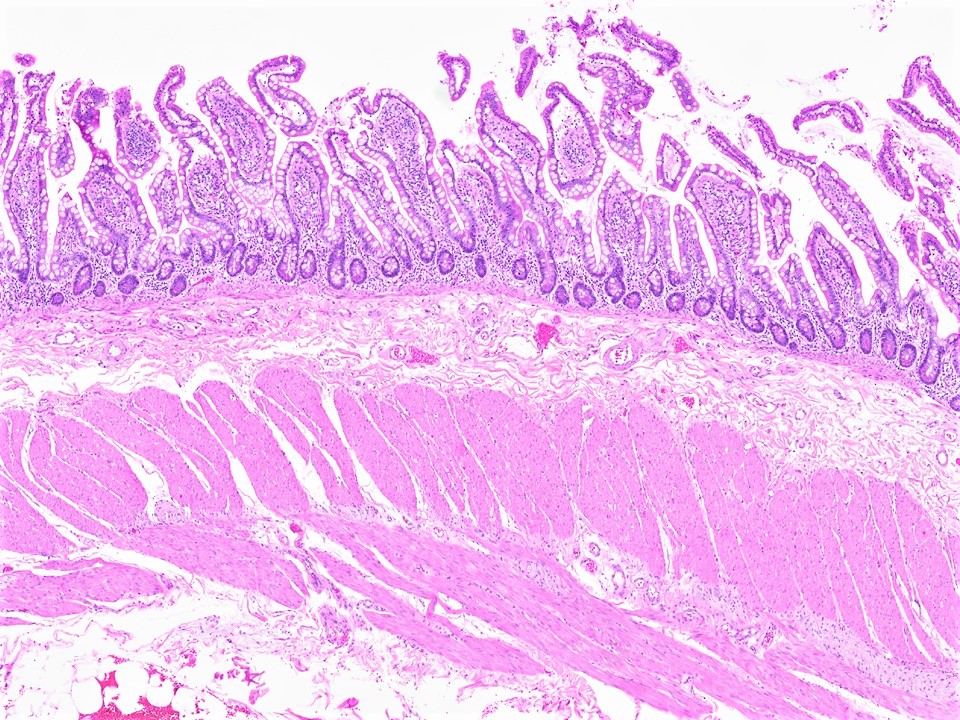
Layers of the Small Intestinal Wall
1. Mucosa
- Villi: Finger-like projections of mucosa into the lumen, 0.5–1.5 mm tall, covered by simple columnar epithelium. Each villus contains a central lacteal (lymphatic capillary), blood capillaries, smooth muscle fibres, and a nerve supply. They are tallest in the jejunum and shortest in the ileum.
- Enterocytes (Absorptive Cells): Tall columnar cells with an apical brush border of microvilli (~3000 per cell). Microvilli increase surface area ~20-fold. Contain digestive enzymes (maltase, sucrase, peptidases) in the glycocalyx.
- Goblet Cells: Mucus-secreting unicellular glands scattered among enterocytes. Increase in number from duodenum → ileum.
- Crypts of Lieberkühn: Tubular glands between the bases of villi that extend to the muscularis mucosae. Contain stem cells (base), Paneth cells (base — secrete defensins/lysozyme), goblet cells, enteroendocrine cells, and immature enterocytes migrating upward.
- Lamina Propria: Loose connective tissue filling the core of villi and surrounding crypts; contains capillaries, central lacteals, smooth muscle, lymphocytes, plasma cells, and mast cells.
- Muscularis Mucosae: Inner circular and outer longitudinal smooth muscle — produces villous movement for absorption.
2. Submucosa
- Duodenum only — Brunner's Glands: Branched tubular mucous glands secreting an alkaline mucus (pH 8–9) to neutralise gastric acid entering the duodenum. Pathognomonic of duodenum.
- Contains Meissner's (submucosal) nerve plexus, blood/lymph vessels.
3. Muscularis Externa
Inner circular and outer longitudinal smooth muscle layers with Auerbach's (myenteric) plexus between them for peristalsis.
4. Serosa / Adventitia
Peritoneum covers jejunum and ileum (serosa); duodenum is largely retroperitoneal (adventitia).
Peyer's Patches
Aggregated lymphoid nodules in the ileal submucosa (occasionally extending into mucosa). Overlying epithelium contains M (microfold) cells that sample luminal antigens and deliver them to underlying lymphocytes. Key site of mucosal immunity. Their presence on a slide confirms ileal tissue.
Regional Differences
- Duodenum: Brunner's glands in submucosa; villi broad and leaf-shaped.
- Jejunum: Tallest, most numerous villi; prominent plicae circulares; richest in goblet cells and crypts.
- Ileum: Shorter villi; Peyer's patches in submucosa; most goblet cells; fewer and lower plicae circulares.
Distinguishing Features on Slide
- Long villi projecting into the lumen — key distinguishing feature from large intestine
- Crypts of Lieberkühn at villus bases
- Brush border visible at high magnification on enterocyte apex
- Brunner's glands in submucosa → confirms duodenum
- Peyer's patches → confirms ileum
References
4 sources- 1
Ross MH, Pawlina W. Histology: A Text and Atlas (8th ed.). Wolters Kluwer; 2020.
- 2
Young B, O'Dowd G, Woodford P. Wheater's Functional Histology (6th ed.). Churchill Livingstone/Elsevier; 2014.
- 3
Junqueira LC, Carneiro J. Basic Histology: Text & Atlas (13th ed.). McGraw-Hill; 2013.
- 4
Eroschenko VP. diFiore's Atlas of Histology with Functional Correlations (13th ed.). Wolters Kluwer; 2017.
Disclaimer: These notes are for educational purposes only and compiled from standard histology textbooks. Clinical interpretation of slides requires a qualified histologist or pathologist.
Ready to test yourself?
Apply what you've learned in the Histology Spotting Test
