Connective Tissue & ECM
Lesson 11 of 16 · Detailed theory + identification points
Points of Identification
4 pointsDetailed Theory
Object: Examination of Connective Tissue Cells and Extracellular Matrix
General Overview
Connective tissue (CT) is characterised by cells scattered in an abundant extracellular matrix (ECM) of fibres and ground substance. Unlike epithelium, CT cells are not tightly packed. Its functions include: structural support, transport of metabolites, defence, energy storage, and repair.
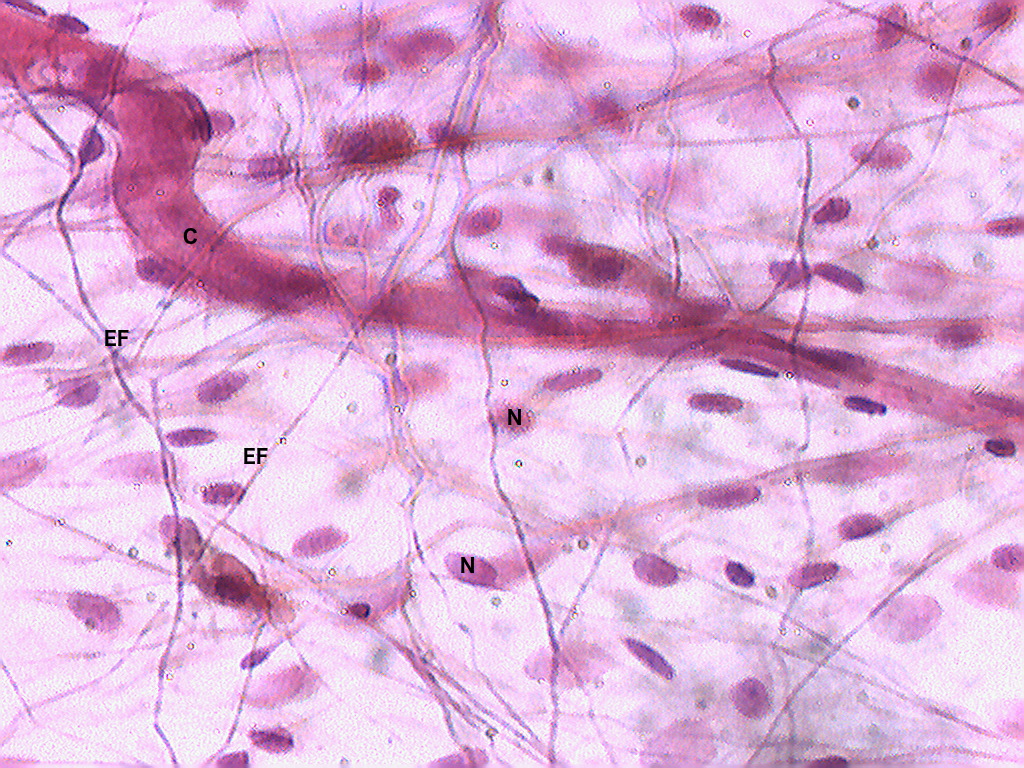
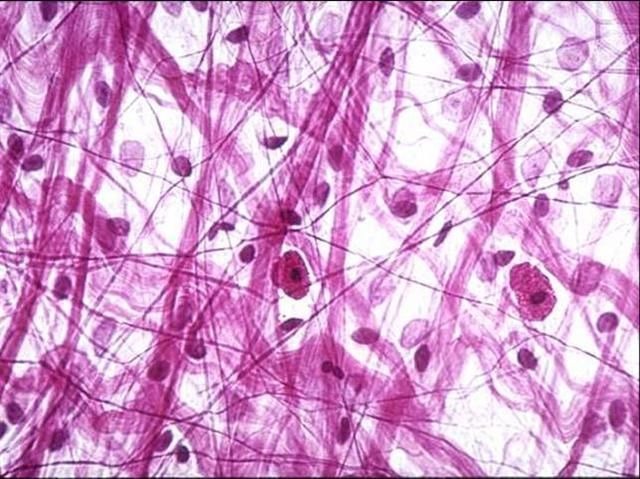
PART A — Connective Tissue Cells
1. Fibroblasts
The most numerous resident CT cell. Active fibroblasts: large, spindle-shaped cells with pale, oval, euchromatic nuclei and a prominent nucleolus; abundant RER (basophilic cytoplasm). Inactive fibroblasts (fibrocytes): smaller, darker, more elongated nuclei. Functions: synthesise all ECM components — collagens, elastin, proteoglycans, glycoproteins. Key cells in wound healing.
2. Histiocytes (Tissue Macrophages)
Derived from blood monocytes (mononuclear phagocyte system). Irregular shape with kidney-shaped or indented nuclei; abundant lysosomes. Functions: phagocytosis of dead cells, microbes, and debris; antigen presentation (express MHC II); secrete cytokines (IL-1, TNF-α). On slides: identified by their kidney-shaped nucleus and phagocytic vacuoles.
3. Mast Cells
Large, ovoid cells found near blood vessels and in loose CT. Cytoplasm packed with large basophilic metachromatic granules (stain purple/red with toluidine blue, Giemsa). Granules contain: histamine, heparin, tryptase, chymase, TNF-α. IgE-receptor (FcεRI) on surface — crosslinking by antigen triggers degranulation (immediate hypersensitivity/allergy). Two types: mucosal mast cells (T-cell dependent) and connective tissue mast cells.
4. Adipocytes (Fat Cells)
White adipocytes: unilocular — single large lipid droplet pushes the nucleus to the periphery. In H&E sections, lipid is dissolved during processing, leaving a large empty space with a peripheral nucleus (signet-ring appearance). Brown adipocytes: multilocular — multiple small droplets; mitochondria-rich; for thermogenesis (abundant in neonates, interscapular region).
5. Plasma Cells
Terminally differentiated B lymphocytes; found in CT wherever antigen exposure is common (gut, respiratory mucosa, lymphoid organs). Histology: oval cells with clock-face (cartwheel) nucleus — heterochromatin in a radial pattern around the nuclear envelope; abundant basophilic cytoplasm (RER for Ig synthesis); prominent pale Golgi area ('Hof' or juxtanuclear clear zone). Produce immunoglobulins (antibodies).
6. Wandering Cells
Cells that migrate into CT from blood as needed:
- Neutrophils: multilobed nucleus; first responders in acute inflammation; phagocytose bacteria
- Eosinophils: bilobed nucleus; large eosinophilic granules; anti-parasitic; modulate allergy
- Lymphocytes: small cells with large dark round nucleus; T and B cells for adaptive immunity
- Monocytes: precursors of tissue macrophages/dendritic cells; kidney-shaped nucleus
PART B — Extracellular Matrix (ECM)
1. Ground Substance
The amorphous, gel-like material filling the spaces between cells and fibres. Appears pale/empty on H&E. Composed of:
- Glycosaminoglycans (GAGs): long unbranched polysaccharides — hyaluronic acid, chondroitin sulphate, heparan sulphate, keratan sulphate. Highly charged; attract water; create a hydrated gel resisting compressive forces.
- Proteoglycans: GAG chains covalently linked to a core protein — aggrecan (cartilage), versican, perlecan. Form large aggregates with hyaluronic acid.
- Glycoproteins: fibronectin (cell adhesion, wound healing), laminin (basement membrane), tenascin, osteopontin. Mediate cell–ECM interactions via integrin receptors.
2. Supporting Tissue Fibres
2a. Collagen Fibres and Their Types
The most abundant protein in the body (~30% total protein). H&E: eosinophilic wavy bundles. Van Gieson stain: red. Masson's trichrome: blue/green.
- Type I (most abundant): thick bundles of high tensile strength; bone, tendon, skin, fascia, dentine, cornea, sclera
- Type II: thin fibres; articular cartilage, vitreous humour of eye; resists compressive forces
- Type III (Reticular fibres): thin (0.5–2 µm), branching fibres forming delicate networks. Stain black with silver (argyrophilic) — silver stain. Found in lymphoid organs, liver (space of Disse), bone marrow, basement membranes, walls of blood vessels and GI tract. Form the scaffolding for soft organs.
- Type IV: non-fibrillar; forms the meshwork of all basement membranes
- Type VII: anchoring fibrils at dermo-epidermal junction
2b. Elastic Fibres
Allow tissues to recoil after stretching. Composed of elastin (core — cross-linked, hydrophobic protein) + fibrillin microfibrils (surrounding sheath). Thinner and more refractile than collagen. Staining: appear indistinct on H&E; specifically stained by orcein (brown), Weigert's resorcin-fuchsin (purple-black), Verhoff's (black). Locations: skin dermis, lung parenchyma (elastin for recoil), walls of elastic arteries (aorta — fenestrated lamellae), ligamentum flavum, vocal cords.
Video Lesson
Connective Tissue & ECM — Histology Video Lesson
Click to play video lesson
References
5 sources- 1
Ross MH, Pawlina W. Histology: A Text and Atlas (8th ed.). Wolters Kluwer; 2020.
- 2
Young B, O'Dowd G, Woodford P. Wheater's Functional Histology (6th ed.). Churchill Livingstone/Elsevier; 2014.
- 3
Junqueira LC, Carneiro J. Basic Histology: Text & Atlas (13th ed.). McGraw-Hill; 2013.
- 4
Eroschenko VP. diFiore's Atlas of Histology with Functional Correlations (13th ed.). Wolters Kluwer; 2017.
- 5
Alberts B et al. Molecular Biology of the Cell (6th ed.). Garland Science; 2015.
Disclaimer: These notes are for educational purposes only and compiled from standard histology textbooks. Clinical interpretation of slides requires a qualified histologist or pathologist.
Ready to test yourself?
Apply what you've learned in the Histology Spotting Test